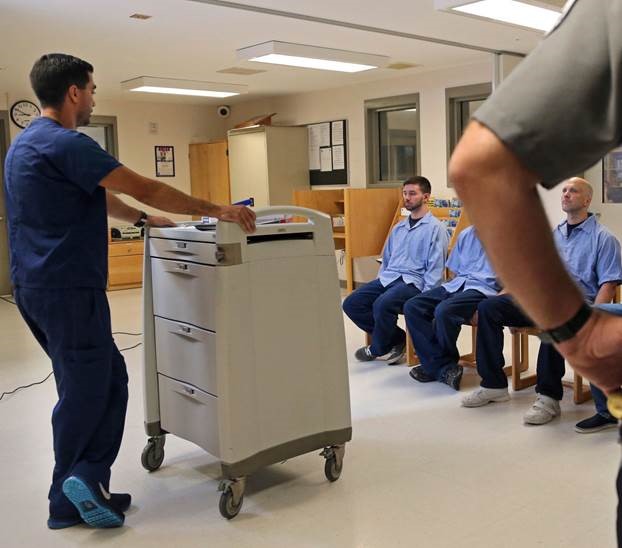
Medication for Addiction Treatment in Correctional Settings
Through the use of medications for addiction treatment (MAT), an individual’s substance use, withdrawal symptoms, and the physiological and psychological cravings can be controlled, enabling the person to begin treatment while in a correctional facility and be released as a person in, or on his or her way to, recovery. Research shows that that the use of MAT for Opioid Use Disorder in correctional settings is a cost-effective and life-saving intervention....